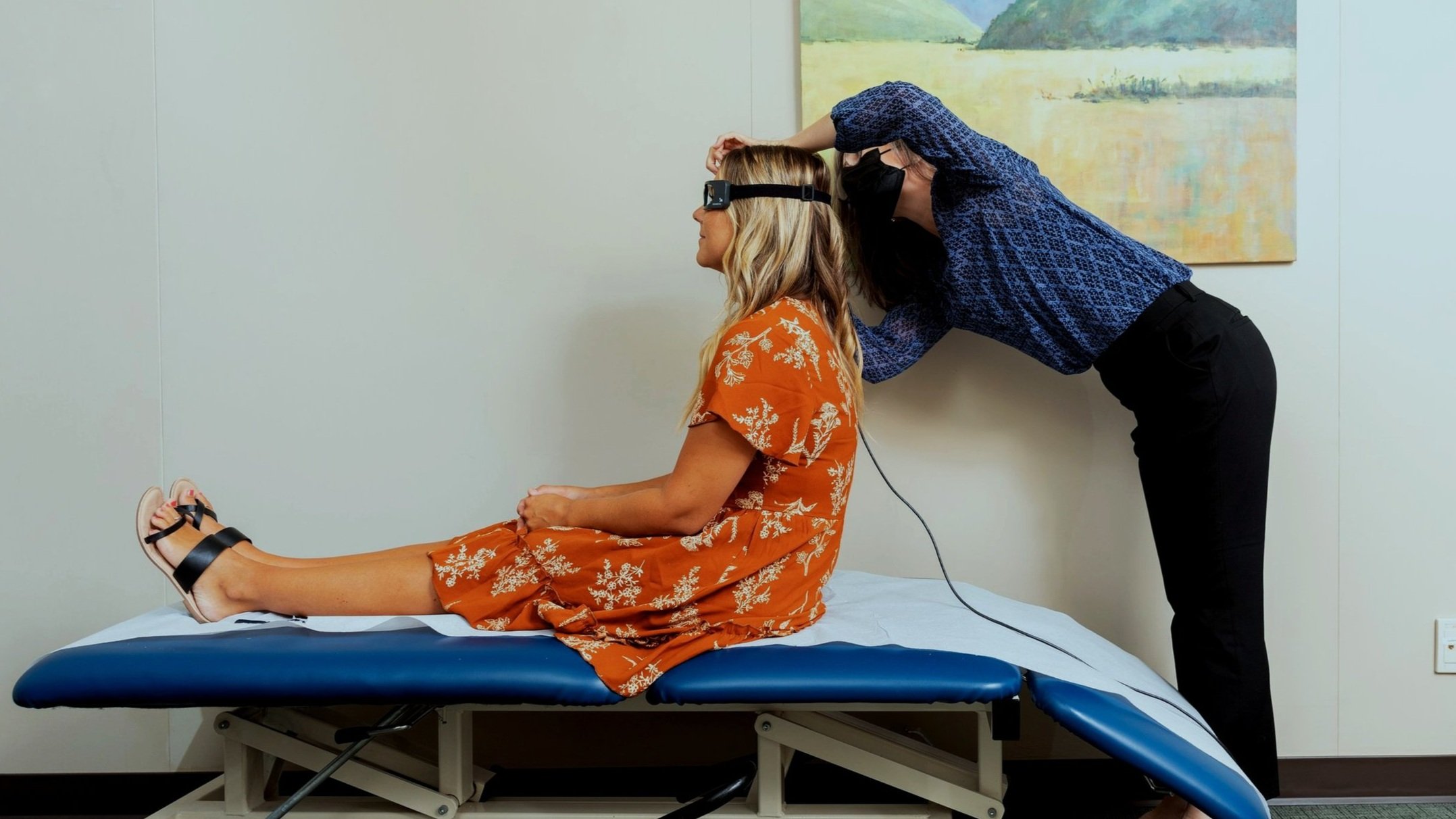
Timely and personalized assessment and treatment for dizziness, vertigo, and balance concerns.
Erica Zaia, MSc, Registered Audiologist
Our Approach
Our private clinic* offers the most modern and accurate tests to assess how the inner ear balance sensors are working and integrating with the eyes, body and brain to maintain balance.
We are able to analyze all five inner ear sensors for balance with our VNG (Videoystagmography), Positional and Positioning Tests, and vHIT (Video Head Impulse Test). Cervical and ocular VEMPs and caloric tests are done when indicated. Each assessment starts with a detailed interview to understand your symptoms and health history, followed by a diagnostic hearing test. This thorough process allows us to interpret results and carefully tailor a treatment plan that can be implemented right away.
*Please note that we are unfortunately unable to bill MSP, ICBC or extended health plans directly.

Erica Zaia
MSc, Registered Audiologist
Erica has performed vestibular testing and rehabilitation for 30 years. She had intense training in vestibular assessment and rehabilitation during her 8 years of education to complete her bachelor’s degree, master’s, and clinical specialization in Audiology. She has worked in a variety of settings, including St. Paul’s Hospital (Vancouver), the Royal National Throat, Nose and Ear Hospital (London, England), and public and private practices in Brazil. She is Clinical Assistant Professor at UBC teaching Audiologists and Physical Therapists, mentor to professionals seeking specialization in the Vestibular field and frequent speaker at conferences raising awareness and sharing knowledge about dizziness, vertigo and balance disorders.
Our Services
-
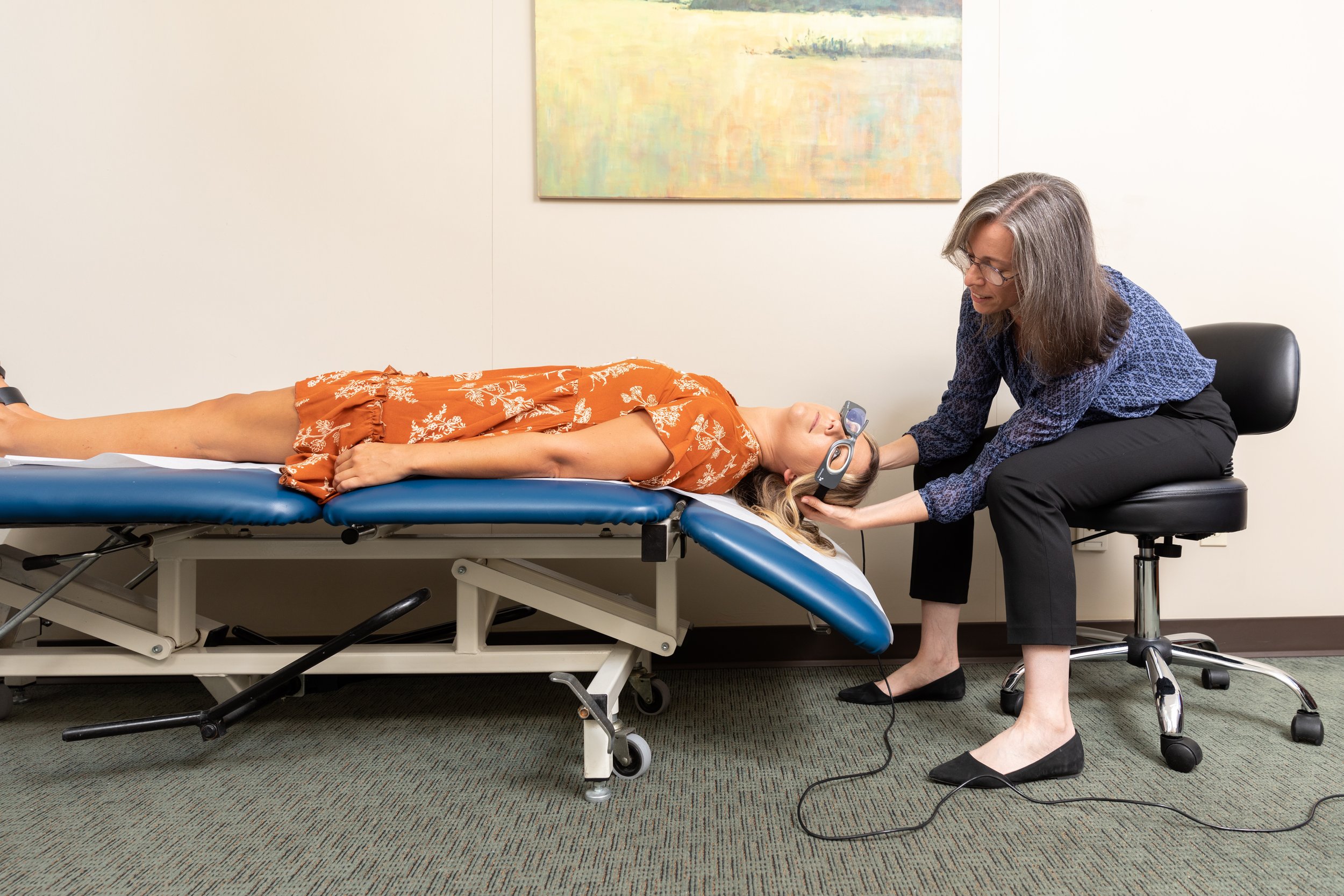
Assessment
Videonystagmography (VNG), VCervical and Ocular VEMPs (Vestibular Evoked Myogenic Potentials) to assess inner ear function and help diagnose vestibular neuritis, BPPV, and central vestibular disorders.
-

Rehabilitation
Vestibular Rehabilitation is proven to be the most effective form of treatment for several forms of vestibular disorders. We perform maneuvers for BPPV and carry on personalized vestibular exercise programs.
-

Hearing Health
We also conduct hearing tests, such as audiometry, speech audiometry and middle ear analysis, in addition to strategies to manage tinnitus and decreased sound tolerance (hyperacusis).

What Our Patients Say
Your local partner in health.
Our office is conveniently located in Vancouver, BC, at 300-3665 Kingsway (corner of Kingsway and Boundary).
Click here to download a PDF file with additional parking and commuting information.

